Development and Update of Guidelines
Introduction
The NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®) are composed of recommendations for the prevention, diagnosis, and management of malignancies across the continuum of care. The library of NCCN Guidelines® currently apply to more than 97% of people living with cancer or anyone at risk for a diagnosis of cancer in the United States. The NCCN Guidelines incorporate real-time updates in keeping with the rapid advancements in the field of cancer research and management. NCCN Guidelines have also been developed for cancer screening and prevention, supportive care issues important to the comprehensive care of patients with cancer, and recommendations regarding cancer care for specific populations (eg, people living with HIV). The NCCN Guidelines are intended to assist all individuals who impact decision-making in cancer care, including physicians, nurses, pharmacists, payers, patients and their families, and others. The development of the NCCN Guidelines is an ongoing and iterative process, which is based on a critical review of the best available evidence and derivation of consensus-driven recommendations by multidisciplinary panels of experts in the field of cancer with the valuable perspective of patients included to the greatest extent possible.
NCCN Guidelines Panel Composition and Roles
The NCCN Guidelines Development Group comprises the NCCN Guidelines Steering Committee, NCCN Guidelines Panel Members, and the NCCN Guidelines Team (NCCN Guidelines staff) that supports the Panels and Guidelines activities. Each NCCN Guidelines Panel includes a Panel Chair, a Vice Chair, and a group of representatives from the NCCN Member Institutions for broad representation of specialties and clinical expertise. Panel membership also includes a patient advocate whenever possible.
The participation of the NCCN Guidelines Steering Committee members, Panel Chairs, and Panel Members is voluntary, and Panel Chairs/Members do not receive compensation for their involvement in the NCCN Guidelines development and update process. The development of the NCCN Guidelines is supported by membership dues from the NCCN Member Institutions, and industry support is not accepted for any direct costs associated with the development of the NCCN Guidelines.
NCCN Guidelines Steering Committee
The Steering Committee provides oversight to the processes and planning of the NCCN Guidelines and comprises representatives from each of the NCCN Member Institutions. Nomination of a Steering Committee member is made by the individual institutions, usually by the institution’s NCCN Board of Directors member. The individual Committee members appoint institutional representatives to each Guidelines Panel, typically in consultation with Panel leadership. Steering Committee members are also responsible for selecting topics for new Guidelines, developing policies for ensuring consistency across Guidelines, overseeing the Institutional Review process (if a given Panel lacks a Panel Member from their institution), ensuring full participation of representatives from their institution in the Guidelines process, and coordinating the implementation of NCCN Guidelines activities or processes within their institutions
NCCN Guidelines Panel Chair and Vice Chair (Panel Leadership)
The Panel Chairs and Vice Chairs are nominated and selected by the leadership of NCCN and the NCCN Guidelines Team, in consultation with the current Panel leadership. The decision considers tenure of service, prior contributions to the Guidelines, multidisciplinary specialty, as well as Member Institution representation in leadership across the spectrum of Panels.
The Panel leadership for each Guidelines Panel provides oversight to the content development activities pertaining to the specific Panel. The Panel leadership also provides input into the selection of representatives for the Guidelines Panels to help ensure the inclusion and participation of relevant clinical expertise within their Panels. The Panel leadership works with the NCCN Guidelines Team to plan the agenda for Panel meetings, presides over these meetings to ensure that all agenda topics are reviewed and discussed, and ensures that formal votes and determinations are made. In addition, the Panel leadership ensures that Panel meetings are conducted in accordance with NCCN policies and procedures and that any Panel Member with a meaningful conflict of interest is excluded from participating in Panel presentations, reviews, discussions, and voting relevant to the area of the conflict of interest.
NCCN Guidelines Panel Members
The Panel Members represent their institutions for all reviews and deliberations of the Panel. The Guidelines Steering Committee member of each institution appoints one of their institution’s members to each Guidelines Panel, typically in consultation with the Panel leadership. The final selection of institutional representatives to each Panel is at the discretion of the institution’s Guidelines Steering Committee member, acting on behalf of their Member Institution. To ensure multidisciplinary representation of the Guidelines Panels, the composition of the Panel represents all of the core medical specialties and clinical expertise involved in the care delivered by the specific Guidelines whenever possible.
In addition, a patient advocate is included as a full Panel Member for each Guidelines Panel whenever possible. Candidates to serve as patient or patient advocate representative(s) are identified by Panel Members, then reviewed and approved by the Panel Chair in consultation with the NCCN Guidelines Team, as needed.
As a general rule, only one individual from a given Member Institution is represented on each Panel. Additional professionals from the same Member Institution may be appointed to the Panel as full members to ensure appropriate representation of clinical expertise. In these cases, each Guidelines Steering Committee member whose institution has no more than one current Panel Member may nominate a candidate, and decisions are made by Panel leadership in conjunction with leadership of the NCCN Guidelines Team.
Panel Members actively participate in the evidence review, deliberations, and votes during the Panel meetings. They may also present data relevant to agenda topics, as assigned by the Panel leadership. Each Member Institution gets one vote even if there is more than one Panel Member on the Panel from a single institution. The patient/patient advocate also gets one vote.
NCCN Guidelines Team
The NCCN Guidelines Team provides planning, development, and procedural support for the Guidelines, and comprises administrative support staff, copyeditors, oncology scientists/writers, coordinators/layout specialists, and the leadership of the NCCN Guidelines Team. The NCCN Guidelines Team works in close collaboration with the Panel to develop and update the Algorithms and accompanying Discussion section to reflect Panel recommendations. The Guidelines Team is also responsible for preparing and posting transparency documents associated with the Guidelines Panel meetings. In addition, members of the NCCN Guidelines Team attend Panel meetings to record/collect meeting minutes and to help clarify the NCCN policies and procedures during the Panel meetings. Staff supporting the relevant NCCN Library of Compendia and Chemotherapy Order Templates applicable to a given Guideline also work with the Guidelines Team to ensure alignment between Guidelines recommendations and these derivative products. The NCCN Guidelines Team and the NCCN Compendium/Chemotherapy Order Templates staff follow a strict firewall policy to shield the NCCN Guidelines development processes from improper influences (see below).
Transparency of the NCCN Guidelines Development Process
To ensure transparency of the NCCN Guidelines development process, the dates for all scheduled NCCN Guidelines Panel meetings, this summary of the Guidelines development process, and the Panel and Guidelines Team Members for each set of Guidelines are posted to the NCCN website. A transparency document is also posted to the NCCN website that captures changes made to the NCCN Categories of Evidence and Consensus or indication of drugs or biologics and requests made through the NCCN submissions process, outcome of requests, references (if applicable), and aggregate results of the Panel vote for each of the changes listed. In addition, all external submission requests are made publicly available on the NCCN website.
Managing Conflicts of Interest
Research contributes to new advances in cancer care and prevention. Many experts and clinical researchers not employed by industry have relationships with industry, which may include receipt of funding for conducting basic or clinical research, or compensation for participation as consultants in advisory boards. These activities often serve to further scientific knowledge, facilitate and accelerate the development of new treatments, and educate both those in industry and academia.
Financial relationships with industry have the potential to introduce conflicts of interest and biases into the NCCN Guidelines development process. Given that the recommendations within the NCCN Guidelines are derived from evaluation of evidence integrated with the clinical experience/judgment and consensus of multidisciplinary panels of experts, it is of paramount importance that NCCN Guidelines Panels reach their decisions in an objective manner without the influence of conflicting interests. In addition, the participation of the NCCN Guidelines Panel Chairs and Panel Members is voluntary, and Panel Chairs/Members do not receive compensation for their involvement in the NCCN Guidelines development and update process. The development of the NCCN Guidelines is supported by membership dues from the NCCN Member Institutions, and industry support is not accepted for any direct costs associated with the development of the NCCN Guidelines.
In order to maintain the integrity of the NCCN Guidelines development process, NCCN has a comprehensive policy for disclosure of financial relationships and for management of potential conflicts of interest. The NCCN policy mandates the disclosure of external financial relationships for all NCCN Guidelines Panel Members and recusal of individuals from deliberations and/or votes when there is a meaningful conflict of interest. Specific disclosure of all relevant financial interests is required for each member of the NCCN Guidelines Panel, including the Chairs, Vice Chairs, and Panel Members, as well as for the NCCN Guidelines Team, members of the NCCN Guidelines Steering Committee, NCCN Senior Leaders, and the NCCN Board of Directors. Categories of disclosure include employment, ownership of equity, ownership interest in a privately held company, royalties, compensation for consultancy, participation in advisory committees, participation in speakers’ bureaus, and receipt of clinical or basic research funding. Restriction of financial relationships for Panel leadership and Panel Members includes limits in absolute dollar amounts received from industry (less than $20,000 from a single entity; and less than $50,000 in aggregate from all sources) and should include the market value of relevant stock ownership. For equity and employment by industry, these standards extend to the individual’s spouse, domestic partner, and dependent children. Panel Chairs/Vice Chairs are not permitted to participate in marketing-focused activities; their involvement in scientific advisory board activities must fall within the dollar amount limits.
Mutual funds, blind trusts, and compensation relating to continuing medical education activities are excluded from the financial limits. The limits also exclude funding of research activities because such funds are typically provided to the Member Institutions rather than to the individual and are used to cover the actual costs of conducting research, often including defrayment of costs normally charged to the participating research subjects. In addition, research remains a core responsibility for academic clinicians. Participation in data safety monitoring boards as part of clinical research is also excluded from the financial limits as this is a key tenet of good clinical practice in research.
NCCN Clinical Practice Guidelines Firewall
NCCN imposes strict policies to shield the NCCN Guidelines development process from improper influences. The “firewall” includes a financial support policy that does not allow NCCN to accept any form of industry or other external financial support for the Guideline development process. The direct costs of the NCCN Guidelines development are supported by membership dues from NCCN Member Institutions. To protect the integrity of the Guidelines development process, Panel Members and NCCN Guidelines Team Members should not be contacted to solicit or suggest changes to Guidelines content. The submission process, as described later, should be used for any requested revisions to Guidelines recommendations. More information regarding NCCN’s firewall policy is available at: https://www.nccn.org/business-policy/business/firewall-policy.
Updates to the NCCN Guidelines
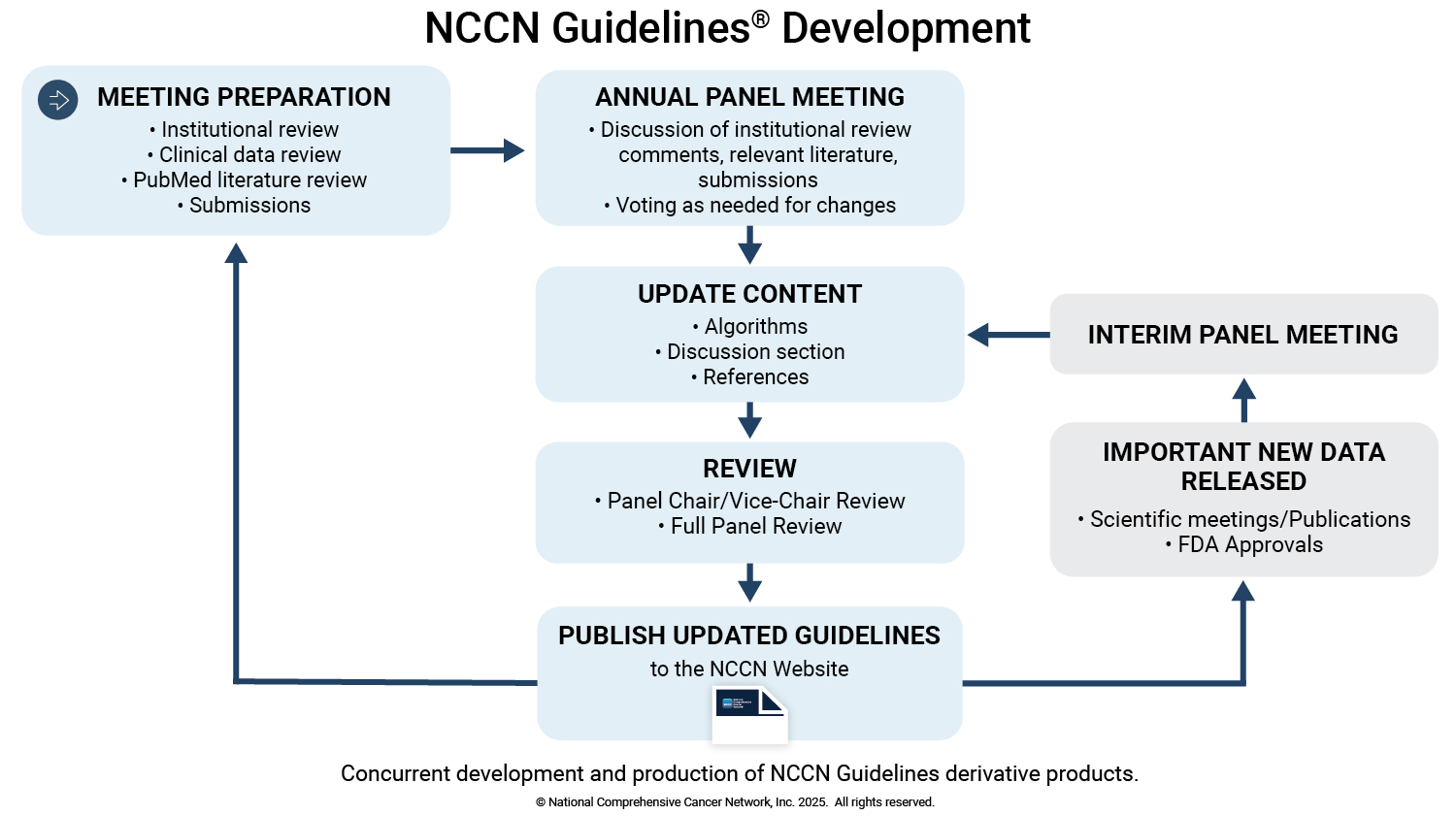
The NCCN Guidelines are reviewed and updated on an ongoing basis to ensure that the recommendations reflect the most current evidence and clinical practice. All NCCN Guidelines are reviewed and updated at least annually. Interim Guidelines updates may also occur based upon new evidence or regulatory approvals of new drugs or biologics that may change clinical practice. The need for an interim Guidelines update is determined by the Panel leadership in conjunction with the NCCN Guidelines Team.
Institutional Review
The annual Institutional Review serves as the cornerstone of the NCCN Guidelines update process (see Figure) and is coordinated by the institutional representative at each Member Institution. During Institutional Review, the NCCN Guidelines are reviewed by the appropriate multidisciplinary specialists at NCCN Member Institutions to identify areas where new data/evidence have changed approaches to care. Responses or comments are gathered and collated by the NCCN Guidelines Team. The responses gathered from the Institutional Review identify important clinical questions, issues, and topics for deliberation at the annual Panel meetings, and serve as one basis for possible revisions or changes to the recommendations contained in the Guidelines.
Literature Review
Prior to the annual update of the Guidelines, the NCCN Guidelines Team performs a search of the PubMed database using appropriate search terms to obtain key literature published since the previous Guidelines update. The PubMed database is used as it remains the most widely used resource for medical literature and indexes peer-reviewed biomedical literature. Articles from additional sources (eg, e-publications ahead of print, meeting abstracts) deemed as relevant to the Guidelines may also be included in the literature review process. Panels are provided with a resulting list of key articles relevant to the Guidelines in advance of Panel meetings to add a rigorous evidence-based review to the NCCN Guidelines development and update process.
Submission Requests
NCCN accepts external requests (submissions) for Panel consideration for changes to Guidelines recommendations. Examples of external requests include submissions from industry, organizations, clinicians/clinical groups, patient advocates, and/or payers. Requests must be submitted at least 4 weeks prior to the scheduled annual Panel meeting to allow the submission materials to be distributed to the Panel leadership and Panel Members for review in advance of the Panel meeting. All submissions are discussed and voted on by the Panel at the Panel meeting. Information on the submission requests process for external parties is available on the NCCN website.
At the time of the Guidelines publication, a transparency document with the actions taken by the Guidelines Panel and aggregate voting results, and the submission request materials are posted to the NCCN website. Also see Transparency of the NCCN Guidelines Development Process, above.
Panel Meetings: Review and Discussion of Evidence
The annual NCCN Guidelines Panel meetings are held as live, in-person meetings or as web conferences. The NCCN Guidelines Team assigned to the specific Guidelines attends the Panel meetings to take minutes of the Panel discussions and record Panel votes. Annual Panel meetings are moderated by the Panel leadership, and attendance by at least 50% of the Panel Members is required for the meetings to proceed.
During the annual Panel meeting, each comment gathered from the Institutional Review, external submissions, or published evidence, and other agenda topics determined by Panel Members and Panel leadership are reviewed and discussed by the Panel. To facilitate the discussions, the Panel leadership or assigned Panel Members may present clinical trial data or other evidence compiled from recently published literature, key presentations from medical society meetings, and/or data from submission requests. When high-level evidence is lacking, the Panels also review lower-level evidence and consider and discuss their clinical experience and expert opinions. Furthermore, evidence of both efficacy and safety of interventions is considered by the Panel. Because most cancer therapies are associated with adverse effects, the overall balance of therapeutic benefit and safety are weighed by the Panels before making their recommendations. The Panel discussion may or may not result in changes to the Guidelines.
A Panel vote is taken for all external submission requests and for changes relating to drugs and biologics (including a change to the NCCN Category of Evidence and Consensus). A Panel vote is also taken in cases where the Panel consensus is unclear. All results of Panel votes relating to drugs, biologics, and external submissions are included in the transparency document, which is posted to the NCCN website (see Transparency and Management of Conflicts of Interest, above).
Interim Panel meetings may be held between annual Panel meetings if needed. These interim meetings are conducted when full Panel discussion is needed to discuss new data that are published or are presented at major medical society meetings or when drugs or biologics are newly FDA approved or granted expanded indications. As with annual Panel meetings, interim meetings are moderated by Panel leadership, attendance by at least 50% of the Panel is required, Panel Members may present evidence on the specific topic, and Panel Members vote on proposed changes as needed. Also see Guidelines Publication, below.
Development of Guidelines Recommendations
Recommendations within the NCCN Guidelines are derived from an integration of a critical evaluation of evidence along with the clinical expertise and consensus of a multidisciplinary panel of experts, especially in situations where high-level evidence does not exist. Panels are charged with evaluating the efficacy of treatment, utility of tests or evaluations, and toxicity of the various interventions. New recommendations and changes to existing recommendations are agreed upon by Panel Members following review and discussion of the evidence during the Panel meetings. The Panel Members deliberate on the interpretation of the clinical evidence and how the evidence should be incorporated into the existing Guidelines. The Panel leadership and Panel Members then develop the wording to denote the specific recommendations within the Algorithms.
The recommendations in the Guidelines are intended to apply to most patients in a particular clinical situation; however, recommendations are not considered to be exhaustive or to apply to all patient situations. Situations expected to arise in less than 5% of cases may be omitted from the Guidelines at the Panel’s discretion.
The NCCN Guidelines represent the breadth of appropriate recommendations for a given clinical situation. As such, a range of options is provided to allow individual clinicians the latitude to select the most appropriate intervention for each patient. In clinical situations where the Panel believes that one or more interventions is likely to be more desirable based on the effectiveness and/or toxicity profile compared with other options, the designation of “preferred” may be used (also see The NCCN Categories of Preference, below). The order in which alternative interventions are listed does not indicate a Panel’s preference, unless specified.
Development of Guidelines Discussion Sections
The Discussion sections provide the scientific rationale and clinical evidence supporting the recommendations outlined in the Algorithm sections of the Guidelines. Additionally, the Discussion sections may expand upon a topic that is only briefly mentioned in the Algorithms (eg, footnotes) or may provide an overview of a subject matter relevant to, but not covered within, the Algorithms. Publications selected from the literature search are also incorporated into the Discussion update. A comprehensive bibliography/reference list (including both published materials and proceedings or abstracts from medical society meetings) on which the Guidelines recommendations are based is included for each Discussion section.
The content of the Discussion sections is generally developed and revised or updated by the NCCN Guidelines Team and Panel leadership. Panel Members may also contribute to the development and/or update of the Discussion sections.
NCCN Guidelines Team and Panel leadership work to update the Discussion sections in a timely manner. NCCN will not delay a Guidelines update to ensure that the Discussion is ready to publish with the Algorithms. Therefore, NCCN publishes Discussion sections with a watermark, indicating the Discussion update is in progress when it has not been updated to be consistent with the current version of the Algorithms. Individual parts of the Discussion may be updated while other sections will have the watermark to indicate that they have not been updated. Each Discussion section includes the date of the last update in a green box on the first page (MS-1).
Guidelines Publication
The NCCN Guidelines Panels hold their annual meetings on a rolling basis from April to December each year. The annual update of the Guidelines is generally extensive and complex, with significant changes to the recommendations, and is usually published within 3 to 6 months of the meeting. This annual version is denoted with a V.1 followed by the version year. The version year does not always correspond to the calendar year because updated Guidelines are posted as quickly as possible following the annual Panel meeting (eg, a Panel that meets in April 2025 might post V.1.2026 in August 2025).
NCCN Guidelines Panels are also responsive to and evaluate new information throughout the year that may have an impact on current clinical practice (eg, new FDA approvals/expanded indications, new peer-reviewed publications). Panels discuss the new information, either via email or web conferences, and may publish interim updates with updated recommendations.
The interim updates generally include a small number of changes to the Algorithm section(s) of the Guidelines or include the addition of the updated Discussion section. These are denoted with V.2, V.3, V.4, etc. for each interim update until the next annual update is published.
All updated Guidelines include a Summary of Guidelines Updates section that lists the changes made for each page in that version.
NCCN Categories for Recommendations
The NCCN Categories of Evidence and Consensus
It is acknowledged that the overall quality of the clinical data and evidence that exist within the field of cancer research is highly variable, both within and across cancer types. Large, well-designed, randomized controlled trials (RCTs) may provide high-quality clinical evidence in some tumor types and clinical situations. However, much of the clinical evidence available to clinicians is based on data from indirect comparisons among randomized trials, phase II or non-randomized trials, or, in many cases, on limited data from multiple smaller trials, retrospective studies, or clinical observations. In some clinical situations, no meaningful clinical data exist, and patient care must be based upon clinical experience and expertise alone.
The NCCN categories for recommendations are based on both the level of clinical evidence available and the degree of consensus within the NCCN Guidelines Panel. The level of evidence depends upon the following factors, which are considered during the deliberation process by the Panel: quality of data (ie, study design and how the results/observations were derived); quantity of data (eg, number of trials, size of trials, clinical observations only); and consistency of data (ie, similar or conflicting results across available studies or observations). The degree of consensus within the Panel is based on the percentage of Panel votes, as shown in the definitions for the NCCN Categories of Evidence and Consensus:
- Category 1: Based upon high-level evidence (≥1 randomized phase 3 trials or high-quality, robust meta-analyses), there is uniform NCCN consensus (≥85% support of the Panel) that the intervention is appropriate.
- Category 2A: Based upon lower-level evidence, there is uniform NCCN consensus (≥85% support of the Panel) that the intervention is appropriate.
- Category 2B: Based upon lower-level evidence, there is NCCN consensus (≥50%, but <85% support of the Panel) that the intervention is appropriate.
- Category 3: Based upon any level of evidence, there is major NCCN disagreement that the intervention is appropriate.
The majority of the recommendations put forth in the Guidelines are category 2A. Where categories are not specified within the Guidelines, the default designation for the recommendation is category 2A.
The NCCN Categories of Preference
In addition to the NCCN Categories of Evidence and Consensus, most Guidelines have systemic therapies stratified by levels of preference. Preference stratification was instituted to clarify Panel preferences for systemic therapies, provide guidance to users of the Guidelines on which recommendations are considered optimal, and continue to provide a wide range of recommendations to meet varying clinical circumstances and patient preferences.
The specific definitions of the NCCN Categories of Preference are:
- Preferred intervention: Interventions that are based on superior efficacy, safety, and evidence; and, when appropriate, affordability.
- Other recommended intervention: Other interventions that may be somewhat less efficacious, more toxic, or based on less mature data; or significantly less affordable for similar outcomes.
- Useful in certain circumstances: Other interventions that may be used for selected patient populations (defined with recommendation).
All recommendations in the NCCN Guidelines are considered appropriate.
NCCN Guidelines with Evidence Blocks
The NCCN Guidelines with NCCN Evidence Blocks™ are intended as a visual representation of five key measures that provide important information about specific recommendations contained within the NCCN Guidelines. These measures are: 1) efficacy of regimen/agent; 2) safety of regimen/agent; 3) quality of evidence; 4) consistency of evidence; and 5) affordability of regimen/agent. The goal is to provide health care providers and patients with information to make informed choices when selecting systemic therapies based upon measures related to treatment, supporting data, and cost. To develop the NCCN Evidence Blocks™, NCCN Panel Members score each measure using a standardized scale from “1” to “5,” with “1” being the least favorable and “5” being the most favorable. Resulting data are analyzed, and final scores are then used to build the 5 x 5 tables that constitute the NCCN Evidence Blocks™ for the interventions. Please click here for more information on NCCN Evidence Blocks™.
NCCN Guidelines: Global Clinical Resources
NCCN Framework for Resource Stratification of NCCN Guidelines (NCCN Framework™)
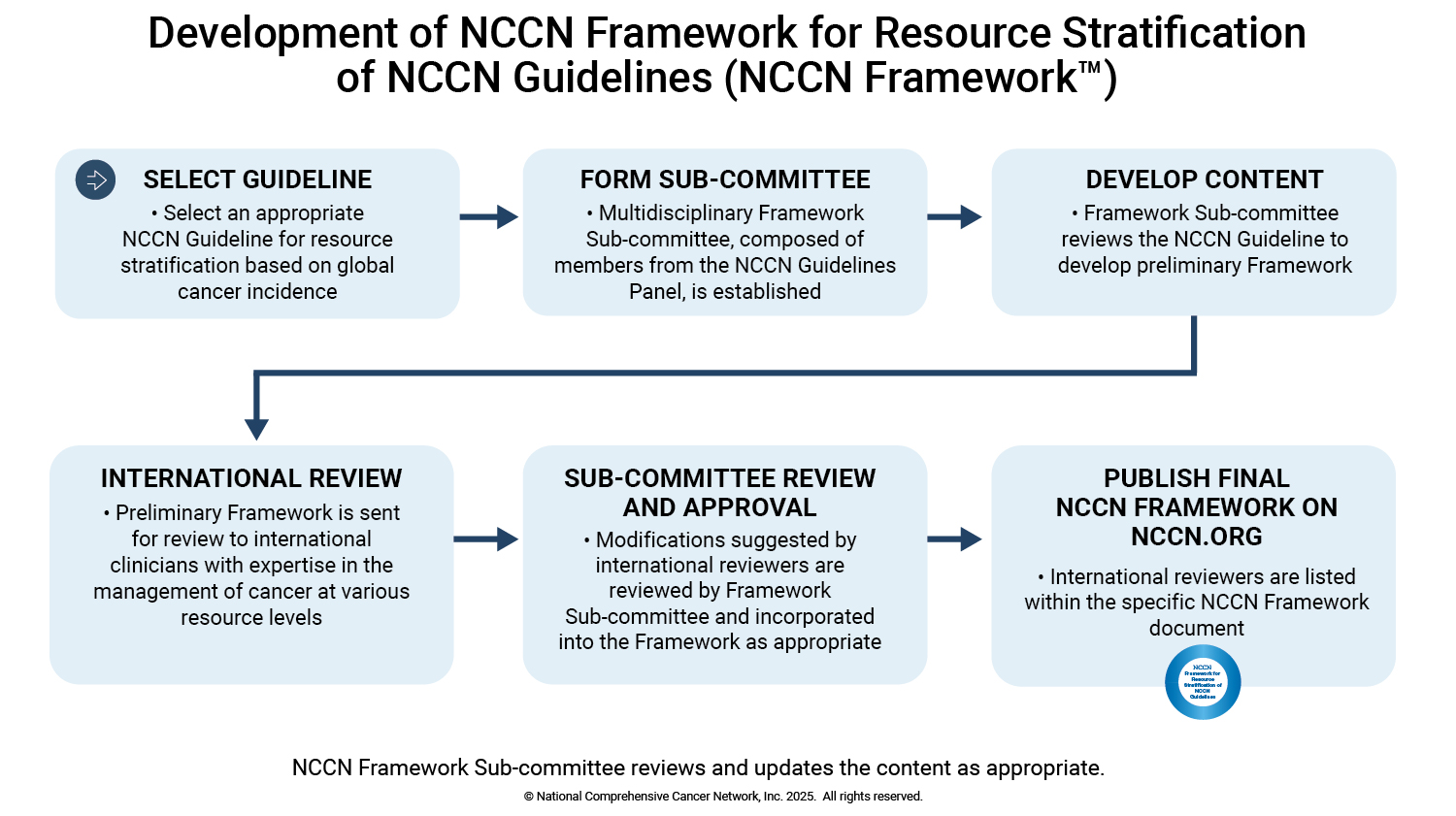
The NCCN Framework™ outlines a rational approach for building cancer management systems to provide the highest achievable cancer care by applying available and affordable services in a logical sequence. The goal of the NCCN Framework™ is to support the use of NCCN Guidelines in countries with limited resources by defining appropriate treatment pathways based on available resources (Basic, Core, and Enhanced)—and to deliver a tool for health care providers to identify treatment options that will provide the best possible outcomes in resource-constrained settings. Each resource level builds on the one before it, with incremental changes to the allocation of resources, providing a structure for improving cancer care. Treatment recommendations applicable at each resource level can be viewed within the context of the NCCN Guidelines.
The NCCN Framework™ is developed by NCCN Framework Subcommittees, which include members of the relevant NCCN Guidelines Panel with experience/knowledge in the care of patients with cancer in countries with limited resources. Following initial development by members of the NCCN Framework Subcommittee, the NCCN Framework™ is reviewed by clinicians from around the world (international review) with expertise in cancer care in resource-constrained settings as identified by NCCN Framework Subcommittee members. The NCCN Framework Subcommittee reviews the input from all international reviewers and amends the NCCN Framework™ as appropriate before publication on NCCN’s website. Please click here for more information on the NCCN Framework™.
International Adaptations of NCCN Guidelines
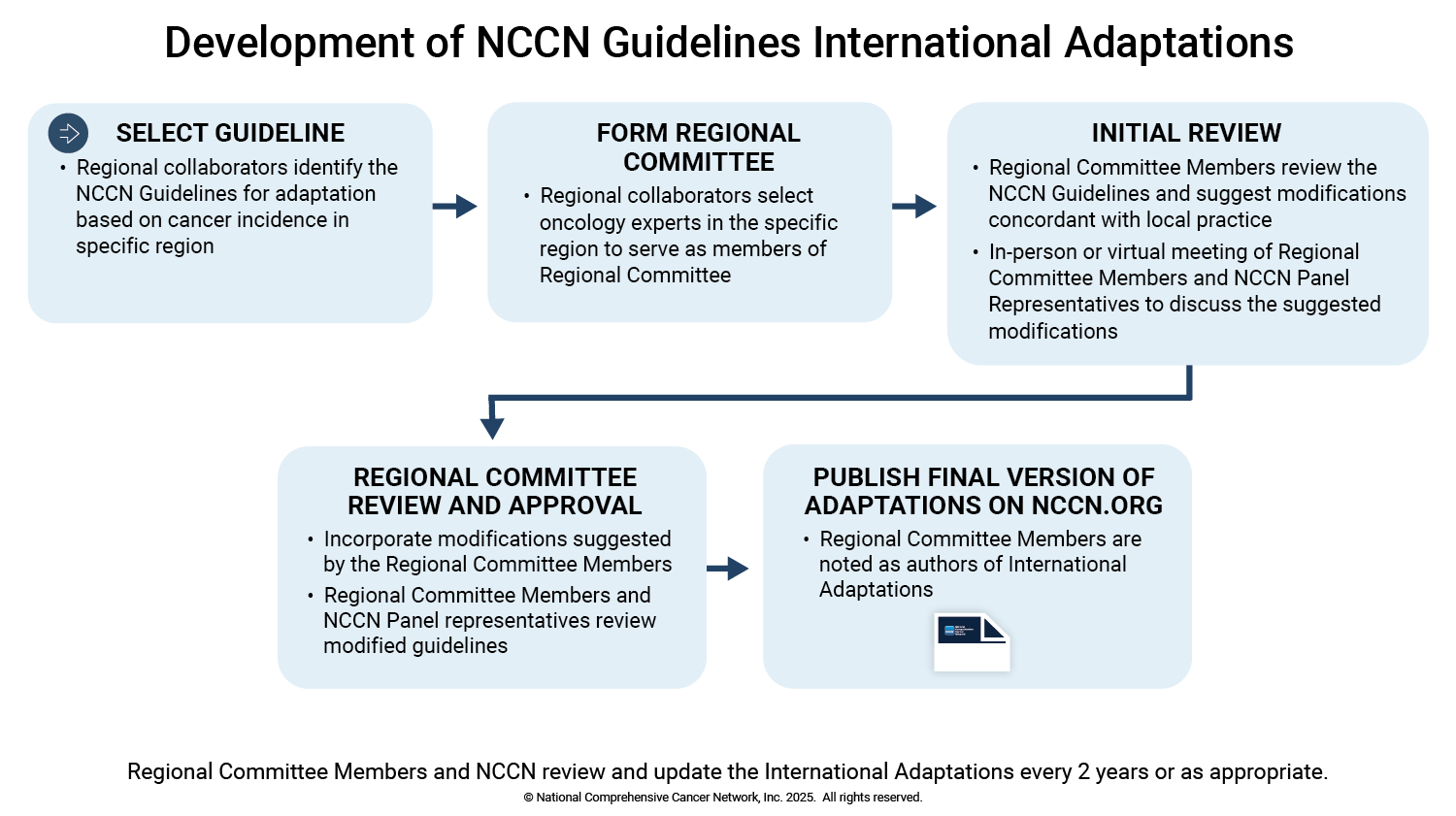
The International Adaptations of the NCCN Guidelines address the availability of resources, metabolic differences in populations, evidence-based regional practice patterns, and regulatory status of health care technologies used in cancer care in a specific country or region. These targeted regional resources are created to combat the rising cancer rates and unique care circumstances in different countries/regions. International Adaptations reflect both the recommendations as delineated in the NCCN Guidelines as well as locoregional variations in care contemplated by the local care environment. Additionally, they may represent both the optimal care that resource-constrained areas aspire to provide and pragmatic approaches that provide effective treatment options in the setting of resource constraints.
International Adaptations are developed by oncology thought leaders in the specific country or region in collaboration with NCCN Guidelines Panel Members to aid clinicians in determining the appropriate and effective care in the specific country or region. These International Adaptions have been used to support improved availability of effective treatment options in specific countries or regions. NCCN has collaborations with the oncologists/oncology organizations in the following countries/regions: Brazil, China, Middle East and North Africa (MENA), Poland, Spain, Sub-Saharan Africa (SSA), and Vietnam.
International Adaptations of NCCN Guidelines are available at: https://www.nccn.org/global/what-we-do/international-adaptations.